Editorially reviewed against guidance and educational materials from:
- PubMed-indexed research
- NIH (National Institutes of Health)
- NINDS (National Institute of Neurological Disorders and Stroke)
- Mayo Clinic
- Cleveland Clinic
This article was created for educational purposes and reflects an evidence-informed editorial review process focused on neuropathy symptoms, vitamin deficiencies, and nerve health support.
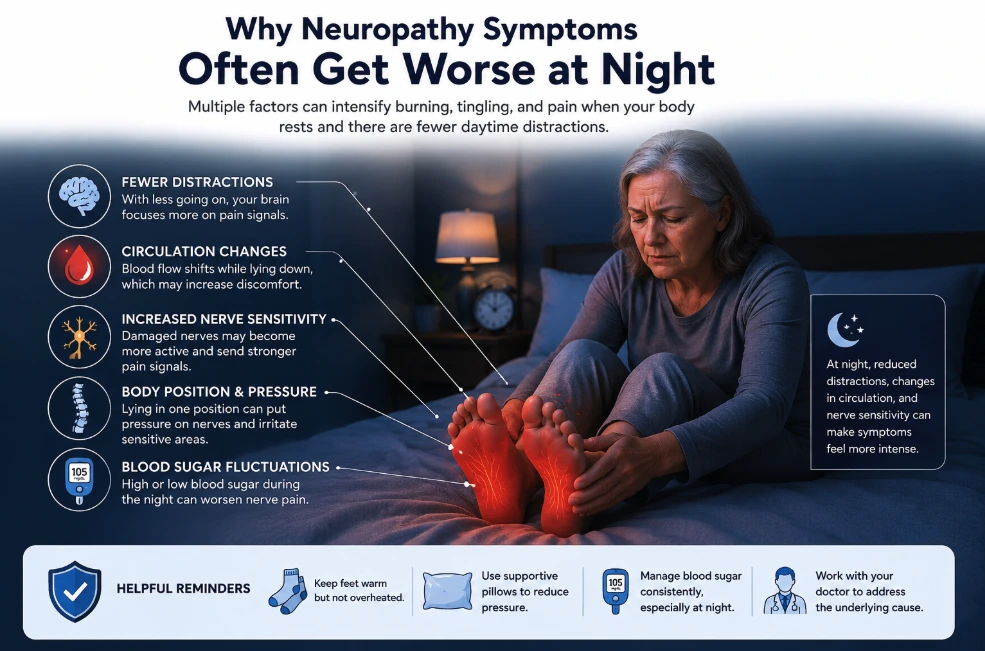
Neuropathy often feels worse at night because there are fewer distractions, circulation changes while resting, increased nerve sensitivity, body-position pressure on irritated nerves, and blood sugar fluctuations that may intensify symptoms after dark. Vitamin B12 deficiency, diabetic neuropathy, poor circulation, and sleep disruption can also contribute to nighttime burning, tingling, and numbness.
Why Does Neuropathy Get Worse at Night?
Mayo Clinic peripheral neuropathy overview, pins-and-needles, numbness, electric-shock sensations, or deep aching pain, most often in the feet and lower legs. Many people notice that these symptoms rise in the evening and peak when they get into bed. That pattern has both neurologic and behavioral explanations.
The first is reduced sensory competition. During the day, your brain is busy processing movement, conversation, work, background noise, and visual input. At night, those distractions disappear. The nerve symptoms may not always be stronger in a biological sense, but they become more noticeable because your brain has less else to focus on.
The second factor is body temperature and circulation. A warm bed, socks, or blankets can intensify burning sensations in some people with neuropathy. Changes in blood flow while lying down may also alter how symptoms are perceived. Some patients describe this as their feet “waking up” in a bad way the moment they rest.
A third issue is positioning. Lying still for long periods can increase pressure on already irritated nerves. If you sleep on one side, cross your ankles, or keep your knees bent for hours, symptoms may flare. This is especially relevant if neuropathy overlaps with spinal issues, nerve compression, or poor circulation.
Common causes behind nighttime neuropathy symptoms
| Possible Cause | How It May Affect Nerves | Common Symptoms |
|---|---|---|
| Diabetes | High blood sugar may damage peripheral nerves over time. | Burning feet, tingling, numbness, nighttime pain |
| Vitamin B12 Deficiency | Low B12 may impair myelin support and nerve communication. | Tingling, balance issues, numbness, fatigue |
| Poor Circulation | Reduced blood flow may worsen nerve discomfort during rest. | Cold feet, burning sensations, leg discomfort |
| Small Fiber Neuropathy | Affects sensory nerve fibers involved in pain perception. | Burning pain, heat sensitivity, nighttime flare-ups |
| Nerve Compression | Pressure on nerves may increase irritation at night. | Shooting pain, numbness, position-related symptoms |
Neuropathy is not one disease. It is a symptom pattern with many possible causes. That matters because relief depends on the driver.
Diabetes and prediabetes are among the most common causes. When blood sugar stays elevated over time, nerves can become damaged, especially in the feet. Nighttime symptoms may worsen if glucose control is inconsistent or if blood sugar dips and rises around bedtime.
Vitamin deficiencies are another major cause, especially low vitamin B12. B12 supports nerve health, myelin integrity, and normal neurologic function. Low levels can contribute to numbness, burning, balance problems, and fatigue. This is one reason many consumers looking for nerve support start by checking whether B12 status has been evaluated properly rather than guessing with random supplements.
Alcohol-related nerve damage, thyroid disorders, kidney disease, autoimmune conditions, infections, and exposure to certain toxins can also contribute. In some cases, neuropathy is called idiopathic, meaning no single cause is identified even after a workup.
Small fiber neuropathy deserves special mention because it often causes burning pain that can feel worse at night. These small nerve fibers help regulate pain and temperature sensation, so even light bedding can feel irritating.
Why does neuropathy get worse at night in some people but not others?
The answer depends on what type of nerves are affected and what else is happening in the body. Someone with primarily numbness may notice little change at night. Someone with painful small fiber neuropathy, poor blood sugar control, low B12, or restless sleep may feel a dramatic increase.
There is also a sleep-pain cycle. Poor sleep lowers pain tolerance. More pain then causes worse sleep. Once that loop starts, nighttime neuropathy can feel progressively harder to manage, even if the underlying nerve damage has not rapidly changed.
Stress can amplify the problem as well. Evening is often when muscle tension rises and people become more aware of bodily symptoms. That does not mean the pain is psychological. It means the nervous system is more reactive under stress, and damaged nerves already have a lower threshold for firing abnormally.
Warning signs that should not be ignored
Some neuropathy symptoms are chronic but stable. Others suggest a need for prompt medical evaluation.
Rapidly worsening numbness, new weakness, foot drop, balance loss, frequent falls, or symptoms spreading quickly up the legs deserve attention. The same is true for neuropathy combined with unexplained weight loss, severe fatigue, bowel or bladder changes, or one-sided symptoms that suggest compression or spinal involvement.
Watch for skin injuries you cannot feel. When neuropathy affects sensation in the feet, cuts, blisters, pressure sores, and burns may go unnoticed and become infected. If your feet feel hot or painful at night but numb during the day, inspection becomes even more important.
Persistent neuropathy can also be a clue that an underlying cause has not been addressed. If no one has checked blood sugar markers, vitamin B12, folate, thyroid function, kidney function, and other relevant labs, that gap matters. Symptom control is helpful, but it should not replace basic investigation.
Relief options that may help at night
The most effective nighttime strategy usually combines trigger reduction with cause-specific support. There is rarely one fix.
Start with temperature control. If heat makes symptoms worse, avoid heavy blankets, overheating the bedroom, or tight socks in bed. Some people do better with breathable bedding and uncovered feet. Others prefer a fan or a cool compress near the feet, though direct ice on numb skin is not a good idea because it can cause injury.
Next, adjust sleep position. If lying flat increases symptoms, try slight elevation or use pillows to reduce pressure on the legs and feet. Avoid positions that compress nerves for long periods. Even small changes in ankle or knee positioning can reduce nighttime irritation.
Glycemic stability matters for patients with diabetes or prediabetes. Large evening carbohydrate loads, skipped meals, or erratic eating patterns may contribute to overnight symptom changes. This is not a call for extreme dieting. It is a reminder that stable blood sugar is part of nerve symptom management.
If deficiency is suspected, targeted nutritional support may be appropriate, especially for vitamin B12. The strongest case for B12 supplementation is when deficiency, low-normal status with symptoms, poor dietary intake, older age, digestive issues, or absorption problems are present. What matters most is the form, dose rationale, and whether there is evidence that the product contains what it claims. This is where analytical supplement review matters more than marketing language.
Certain topical approaches may also help some patients. Creams or gels designed for localized discomfort can reduce surface sensitivity in the feet before bedtime. Results vary, and they are symptom-focused rather than corrective, but they may improve comfort enough to support sleep.
Gentle movement can help too. A short walk, calf stretches, or ankle mobility work in the evening may improve circulation and reduce the transition from daytime activity to nighttime flare. Overdoing exercise late at night, however, can backfire if it increases inflammation or cramps.
| What May Worsen Symptoms | What May Help |
|---|---|
| Overheating during sleep | Cooler room temperature |
| Tight socks or heavy blankets | Breathable bedding |
| High evening sugar intake | Stable blood sugar habits |
| Poor sleep positioning | Leg elevation and pillow support |
| Ignoring vitamin deficiencies | Proper medical evaluation |
| Long periods without movement | Gentle evening stretching |
What to look for in a neuropathy support supplement
People searching for relief often end up comparing nerve support formulas. That is reasonable, but the label should be judged clinically, not emotionally.
A credible formula should have ingredients with a plausible role in nerve health, such as vitamin B12 when deficiency risk exists, along with transparent dosing. It should avoid proprietary blends that hide ingredient amounts. Manufacturing quality, third-party testing, and clear contraindication language also matter.
Be careful with products that imply they can reverse all neuropathy causes. That is not realistic. A supplement may support normal nerve function, help correct a deficiency, or contribute to symptom management in some users, but it is not a substitute for diagnosis when red-flag symptoms are present.
For readers who regularly compare encapsulated health products, the most useful question is not “What is the most advertised formula?” It is “Which product has the best evidence-to-claim ratio for my likely cause?” That is a more reliable way to spend money.
When self-management is not enough
If neuropathy is disrupting sleep several nights a week, progressing, or affecting walking and daily function, self-care alone may not be enough. Medical review helps clarify whether the issue is metabolic, nutritional, autoimmune, compressive, or something else entirely.
This is especially relevant if symptoms began suddenly or if numbness is replacing pain. Many patients assume less pain means improvement, but increasing numbness can reflect advancing nerve dysfunction rather than recovery.
A careful workup also reduces the risk of chasing the wrong solution. Buying multiple supplements without knowing whether the problem is B12 deficiency, poor glucose control, alcohol-related damage, or spinal compression is not efficient or evidence-based.
Practical next steps for better nights
If nighttime neuropathy is becoming a pattern, start by tracking when symptoms peak, whether heat triggers them, and whether they relate to meals, alcohol, sleep position, or activity level. That information can make medical visits more useful and can help you identify patterns quickly.
Then focus on the basics that actually move the needle: foot inspection, stable blood sugar if relevant, correcting known deficiencies, better sleep positioning, and careful supplement selection based on evidence rather than hype. For many people, relief comes from narrowing the cause and removing aggravators, not from chasing dramatic promises.
Nighttime neuropathy is frustrating because it hits when you most need rest. But the pattern often contains clues. If you treat those clues as useful data rather than random discomfort, you are much more likely to find relief options that make sense and hold up under scrutiny.
Frequently Asked Questions
Why do my feet burn more at night?
Burning feet may feel worse at night because there are fewer distractions, circulation changes become more noticeable during rest, and damaged nerves can become more sensitive in warm environments or while lying down.
Can low vitamin B12 cause nighttime tingling?
Low vitamin B12 levels may contribute to tingling, numbness, burning sensations, and nerve-related symptoms in some individuals, especially when deficiency affects nerve communication and myelin support.
Why does neuropathy feel worse when lying down?
Some people notice increased symptoms while lying down because body position, pressure on irritated nerves, circulation shifts, and reduced movement can make nerve discomfort easier to feel.
Can poor circulation make neuropathy worse at night?
Poor circulation may contribute to nighttime burning, numbness, or discomfort in some individuals, particularly when combined with diabetes, inactivity, or existing nerve damage.
When should nighttime neuropathy be medically evaluated?
Rapidly worsening symptoms, weakness, falls, severe numbness, bladder changes, or unexplained neurological symptoms should be evaluated by a healthcare professional promptly.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended as medical advice. Dietary supplements are not a replacement for professional medical diagnosis or treatment. Always consult with a qualified healthcare professional before starting any new supplement, especially if you have pre-existing medical conditions or are taking prescription medications. Individual results may vary.
- What “Clinically Studied” Means in Supplements - May 12, 2026
- Guide to Clinical Ingredient Dosing - May 12, 2026
- Third-Party Testing vs Marketing Claims - May 11, 2026
