Editorially reviewed against guidance and educational materials from:
- PubMed-indexed research
- NIH (National Institutes of Health)
- NINDS (National Institute of Neurological Disorders and Stroke)
- Mayo Clinic
- Cleveland Clinic
This article was created for educational purposes and reflects an evidence-informed editorial review process focused on neuropathy symptoms, vitamin deficiencies, and nerve health support.
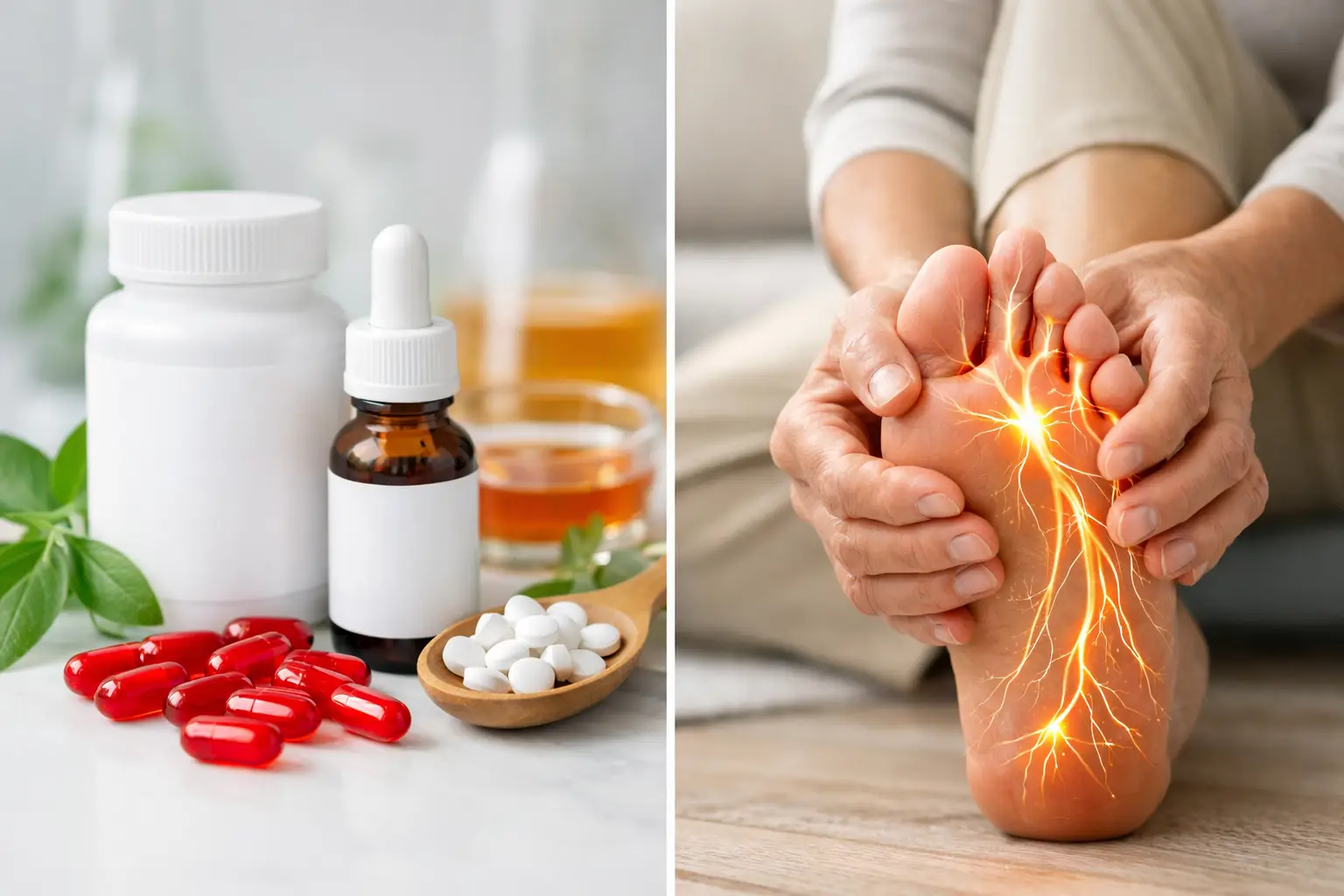
Numb toes, burning feet, and pins-and-needles in the hands are often dismissed as generic nerve damage. But when it comes to B12 deficiency vs diabetic neuropathy, that assumption can be misleading — and even risky. The overlap in symptoms is significant, but the underlying causes and treatment paths are very different. If you have diabetes, prediabetes, or persistent fatigue with nerve symptoms, understanding this distinction is critical for choosing the right intervention.
Important: Treating the wrong cause of nerve damage can delay recovery and worsen long-term outcomes. That’s why distinguishing between B12 deficiency and diabetic neuropathy is not just technical — it directly affects treatment success.
Why b12 deficiency vs diabetic neuropathy gets confused
Both conditions can affect peripheral nerves. Both can cause tingling, numbness, burning pain, balance changes, and reduced sensation in the feet. In practice, many people assume diabetic neuropathy first, especially if blood sugar has been high or diabetes is already on the chart.
That assumption is not always wrong, but it can be incomplete. Vitamin B12 deficiency can produce a neuropathy that looks very similar, and in some cases both problems exist at the same time. This is one reason clinical evaluation matters more than guesswork or buying a random nerve support formula.
There is also an important consumer point here. People shopping for B12 supplements are often trying to solve fatigue, brain fog, or nerve symptoms quickly. A quality B12 product may be useful if deficiency is present, but it is not a stand-in for testing. Without evidence of low or borderline B12 status, supplementation becomes less targeted and the results are harder to interpret.
What B12 deficiency neuropathy usually looks like
Vitamin B12 is essential for nerve function, red blood cell production, and DNA synthesis. When levels fall low enough, the nervous system can be affected. The pattern is often gradual. People may notice tingling in the feet first, then worsening numbness, clumsiness, reduced vibration sense, or trouble with balance.
If you’re still unsure how B12 directly affects nerve repair and neurological symptoms, see this detailed explanation: how vitamin B12 supports nerve health and recovery.
Clinical research has consistently shown that vitamin B12 plays a critical role in maintaining the integrity of the myelin sheath, which protects nerve fibers and supports proper neurological signaling.
B12 deficiency can also come with clues that diabetic neuropathy does not always explain well. Fatigue, pale skin, shortness of breath with exertion, memory complaints, sore tongue, and anemia may appear alongside the nerve symptoms. Not every patient has all of these, and some have neurological symptoms even before obvious anemia appears.
Risk factors matter. Low B12 becomes more likely with long-term vegetarian or vegan diets without supplementation, poor absorption, certain stomach or intestinal disorders, older age, heavy alcohol use, or long-term use of medications that reduce B12 absorption. People with diabetes may also be at higher risk of B12 deficiency, which complicates the picture further.
What diabetic neuropathy usually looks like
Diabetic neuropathy is nerve damage linked to chronic high blood sugar and related metabolic stress. The most common form is distal symmetric polyneuropathy, which typically starts in the feet and moves upward in a stocking pattern. Burning pain at night, numbness, reduced protective sensation, and foot injuries that go unnoticed are common warning signs.
According to the American Diabetes Association, diabetic neuropathy is one of the most common complications of long-term uncontrolled blood sugar, highlighting the importance of distinguishing it from other causes of nerve damage such as vitamin deficiencies.
In both B12 deficiency and diabetic neuropathy, symptoms often start in the feet and gradually progress upward, which is why early-stage nerve damage is frequently overlooked. If you want to better understand how these early symptoms develop and what they may indicate, see this detailed guide: early signs of nerve damage from vitamin deficiency.
The history often supports the diagnosis. Long-standing diabetes, poor glucose control, metabolic syndrome, kidney disease, and other diabetes complications increase the odds. Some people also develop autonomic symptoms such as dizziness on standing, digestive changes, sweating abnormalities, or sexual dysfunction.
The key limitation is that symptom pattern alone is not enough. A person with diabetes can still have B12 deficiency. In fact, mixed neuropathy is one of the more overlooked scenarios in routine care.
B12 deficiency vs diabetic neuropathy: key differences
The cleanest distinction is cause. B12 deficiency neuropathy is driven by inadequate vitamin availability or absorption. Diabetic neuropathy is driven mainly by glucose-related nerve injury. That sounds simple, but real-world cases are often messy.
B12 deficiency becomes more likely when nerve symptoms come with fatigue, anemia, balance problems, cognitive changes, or known nutritional risk. Diabetic neuropathy becomes more likely when there is a clear diabetes history, elevated A1C, and a classic foot-predominant pattern that developed over time.
Another practical difference is reversibility. If B12 deficiency is identified early and corrected, improvement can be meaningful and sometimes substantial. If deficiency has been prolonged, recovery may be partial and slow. Diabetic neuropathy can also improve symptomatically, especially with tighter metabolic control and early intervention, but established nerve damage is often harder to reverse.
This is why timing matters. Waiting months while self-treating numbness with a general supplement stack can reduce the chance of a better outcome.
B12 deficiency vs diabetic neuropathy: quick comparison
| Factor | B12 Deficiency Neuropathy | Diabetic Neuropathy |
|---|---|---|
| Main cause | Low or poorly absorbed vitamin B12 | Chronic high blood sugar |
| Onset | Gradual, can include fatigue and anemia | Gradual, strongly linked to diabetes history |
| Common symptoms | Tingling, numbness, balance issues, brain fog | Burning pain, numbness, loss of sensation in feet |
| Reversibility | Often reversible if caught early | Harder to reverse once established |
| Key test | Vitamin B12, MMA, homocysteine | A1C, blood glucose levels |
The tests that actually help
If the question is b12 deficiency vs diabetic neuropathy, the answer usually comes from basic clinical data, not symptom guessing. Blood work is central. A serum B12 level is the usual starting point, but borderline results can be misleading. In those cases, methylmalonic acid and sometimes homocysteine can help clarify functional B12 deficiency.
A complete blood count may show macrocytic anemia, although its absence does not rule out neurological B12 deficiency. For diabetic neuropathy, fasting glucose, A1C, kidney markers, and a full metabolic review are often relevant. A clinician may also check thyroid function, folate, and other causes of neuropathy because not all numbness is from diabetes or B12 issues.
Neurological exam findings matter as much as lab work. Vibration sense, reflexes, gait, proprioception, and foot sensation can help narrow the cause. In selected cases, nerve conduction studies may be useful, especially when the pattern is atypical or rapidly progressive.
When B12 supplementation makes sense
If testing confirms low or borderline B12, supplementation is rational and often necessary. The better question is not whether B12 is “good for nerves” in general, but whether the form, dose, and delivery method fit the actual deficiency risk.
Oral high-dose B12 can work well for many people, even with some absorption limitations, while others may need clinician-guided treatment. Methylcobalamin and cyanocobalamin are the most common forms on the market.
If you’re comparing supplement options at this stage, it’s important to understand how different B12 forms affect nerve-related symptoms and absorption. This detailed comparison breaks it down clearly: methylcobalamin vs cyanocobalamin for nerve pain.
For supplement shoppers, quality control, transparent labeling, dose accuracy, and unnecessary additive load matter more than flashy claims.
A B12 supplement is more likely to deliver value when there is a defined reason to use it: confirmed deficiency, low-normal levels with compatible symptoms, dietary insufficiency, or an established absorption risk. If the true driver is diabetic neuropathy without B12 deficiency, B12 alone may not produce the result the buyer expects.
That is where an evidence-based review approach helps. Before spending on a premium encapsulated product, look for clear dosing information, third-party quality standards when available, and realistic claims. Products that imply they “repair” all nerve damage are overselling.
Can both happen at once?
Yes, and this is one of the most clinically relevant points. A person with diabetes may develop neuropathy from blood sugar exposure and also have B12 deficiency at the same time. In that setting, the symptoms can seem worse, recovery can be slower, and treatment needs to address both problems.
This overlap is one reason some clinicians check B12 status more carefully in patients with diabetes who develop new numbness, burning, or balance issues. For the consumer, the takeaway is simple: if you already have diabetes, do not assume every nerve symptom is automatically diabetic neuropathy.
What supplement buyers should do before choosing a product
If your main question is whether a B12 supplement is worth buying, first determine whether low B12 is plausible. Look at your diet, digestive history, age, and lab work if available. If symptoms include numbness, weakness, balance problems, or persistent fatigue, testing is the fastest way to avoid a mismatched purchase.
Next, evaluate the formula. A useful B12 product should state the exact form and dose clearly, avoid proprietary blends that hide amounts, and fit your needs realistically. Very high doses are not automatically better for every buyer. What matters is whether the product addresses a documented gap.
Finally, set expectations. Nerve symptoms do not always improve quickly, even when the right deficiency is corrected. If diabetic neuropathy is present, glucose management, foot care, and broader metabolic control remain central. Supplements may support a plan, but they do not replace diagnosis.
Final verdict on b12 deficiency vs diabetic neuropathy
Major medical institutions such as the Mayo Clinic and the Cleveland Clinic emphasize that identifying the root cause of neuropathy is essential for effective treatment, since different conditions require fundamentally different approaches.
For most readers, the safest takeaway is this: treat b12 deficiency vs diabetic neuropathy as a testing question, not a guessing game. The symptoms overlap too much to rely on internet pattern-matching alone, and the best supplement choice depends on the cause. If B12 is low, a well-formulated supplement can be a practical and evidence-based part of the solution. If the real issue is diabetic neuropathy, you need a broader plan than B12 alone.
The smartest health purchase is often not the most heavily marketed bottle – it is the product that matches a verified need.
If you’re still unsure which type of nerve issue you’re dealing with, reviewing early symptoms and understanding supplement differences can help you make a more informed decision before choosing any product.
Frequently Asked Questions
What is the difference between B12 deficiency and diabetic neuropathy?
B12 deficiency neuropathy is caused by low or poorly absorbed vitamin B12, while diabetic neuropathy results from long-term high blood sugar damaging the nerves. Although symptoms like tingling, numbness, and burning pain can look similar, the underlying cause — and treatment — is completely different.
Can B12 deficiency cause nerve damage similar to diabetes?
Yes. Vitamin B12 deficiency can cause nerve damage that closely mimics diabetic neuropathy. Symptoms often start with tingling in the feet, numbness, balance issues, and reduced sensation, which is why many people misinterpret the cause early on.
How do you test for B12 deficiency vs diabetic neuropathy?
Doctors typically use blood tests such as vitamin B12 levels, methylmalonic acid (MMA), and homocysteine to detect deficiency. For diabetic neuropathy, A1C and blood glucose levels are key. A neurological exam is often needed to confirm the cause.
Can B12 supplements reverse nerve damage?
If nerve damage is caused by B12 deficiency and treated early, symptoms can improve significantly. However, long-term or severe damage may not fully reverse, which is why early diagnosis is critical.
Should people with diabetes check their B12 levels?
Yes. People with diabetes have a higher risk of B12 deficiency, especially when using certain medications. Checking B12 levels can help prevent worsening nerve damage or misdiagnosis.
Medical Disclaimer: The information provided in this Review is for educational purposes only and is not intended as medical advice. Dietary supplements are not a replacement for professional medical diagnosis or treatment. Always consult with a qualified healthcare professional before starting any new supplement, especially if you have pre-existing medical conditions or are taking prescription medications. Individual results may vary.
- What “Clinically Studied” Means in Supplements - May 12, 2026
- Guide to Clinical Ingredient Dosing - May 12, 2026
- Third-Party Testing vs Marketing Claims - May 11, 2026